As emergency room doctors nationwide plead for help to ease patient overcrowding, the one federal program that could fix the crisis is poised to lose funding.
Across the U.S., ER patients who need to be hospitalized find themselves stuck in hallways or waiting rooms, sometimes for days or weeks, before they are able to get further care.
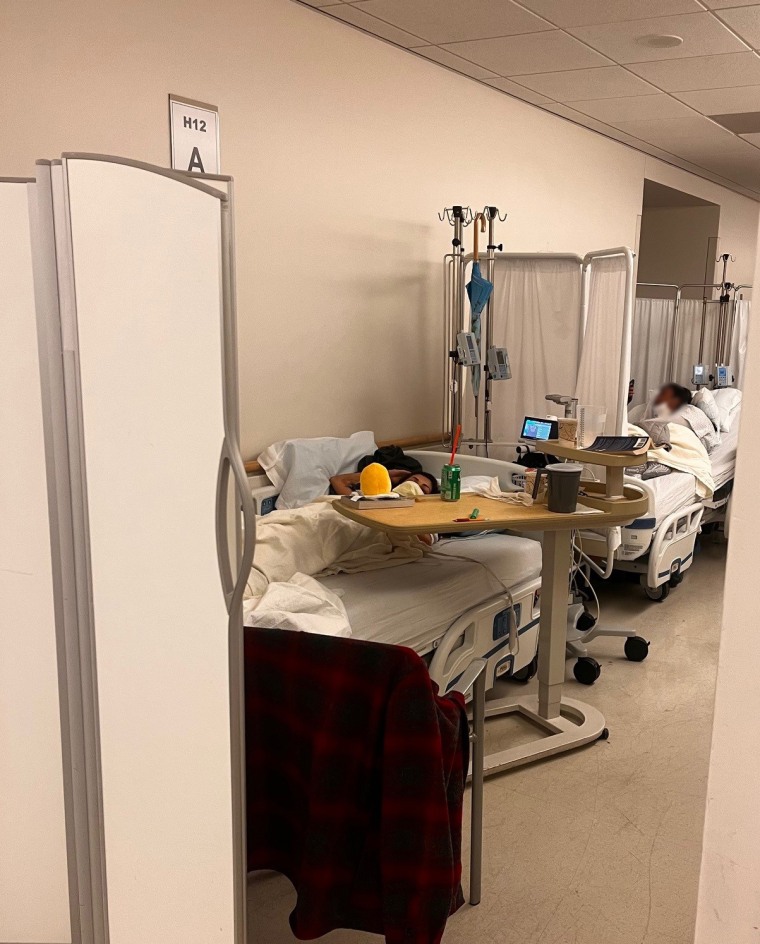
Marissa Long, 30, spent three days and four nights on a gurney in a busy Los Angeles ER hallway last March, separated from other sick patients just a few feet away by a thin fabric curtain.
Long, a heart transplant recipient, was showing signs of possible organ rejection: trouble breathing and falling blood pressure. She needed to be admitted to the hospital, but there were no beds available.
“People were coughing and vomiting,” Long said. “I already have a low immune system. I was scared to get sick.”
Last summer in Bangor, Maine, Michael Day had heard of ER hallways full of sick patients, hacking and sneezing; people left sitting for days on hard, plastic waiting room chairs.
He did not want to go to the emergency room, although the 75-year-old had no choice. Following a diagnosis of advanced esophageal cancer, he was rapidly declining. He was weak and jaundiced. His blood pressure was plummeting.
Without no available room in the hospital, Day found himself stuck in the ER, twice.
On one visit, Day developed a bed sore from remaining stationary for more than 26 hours. During another, the ER staff started him on an IV to replenish his fluids and hooked him up to a blood pressure monitor while he waited to be seen by a doctor.
Once again, hours ticked by.
Day’s wife, Kathy — a former ER nurse — said they were there so long that the batteries in her husband’s blood pressure monitor eventually died. His IV ran out and dried up. The staff on duty, Kathy Day said, did not notice.
At that moment, Kathy Day uttered the sentiment echoed by countless ER patients across the country: “This is bulls—.”

ER patients waiting for beds that don’t exist
Emergency medical care is meant for one of two things: Treat a person quickly and send them home — stitch up a deep cut, perhaps, or determine that a high fever isn’t a life-threatening infection, for example; or get the patient admitted into the hospital for further care.
Because America’s health care system as a whole is woefully understaffed to care for an aging population rife with chronic illnesses, or to meet increasing needs for mental health services, patients show up in the ER and, without any place else to go, stay in the ER.
“There are fewer nursing home beds. There are fewer rehab beds. There are fewer psychiatric beds,” said Dr. Ali Raja, deputy chair of emergency medicine at Massachusetts General Hospital in Boston. “Our overall length of stay for inpatients has gone up. Since those patients are staying longer in the hospital, we end up having more boarders in the emergency department.”
Ninety-seven percent of ER doctors said they experienced patient boarding times of more than 24 hours, according to a November 2022 survey by the American College of Emergency Physicians.
More than a quarter, 28%, of the ER doctors said patients were forced to stay in the ER for more than two weeks before getting a hospital bed.
“There have been instances where patients are literally waiting for several weeks to months,” Dr. Aisha Terry, president of the American College of Emergency Physicians, said during a briefing in October with reporters. “Patients are leaving early, or dying waiting.”

Rising health care costs have forced health systems nationwide — often in rural areas — to shutter hospitals and other medical facilities in recent decades, according to the American Hospital Association. Elder care centers have also been affected, especially during the pandemic. A report from the Bureau of Labor Statistics shows that the number of workers in nursing homes and other care facilities fell by 410,000 between February 2020 and November 2021.
Dr. Joseph Tennyson, president of the Massachusetts chapter of the American College of Emergency Physicians said he recently worked an ER shift in which he had patients on oxygen support “waiting hours for an ICU bed that didn’t exist.”
Raja said his ER has been operating at a level dubbed “capacity disaster” — with at least 45 patients boarded at a time — for at least a year. On Jan. 11, the Massachusetts General Hospital ER reached an unfathomable level of boarded patients: 103. The situation prompted the hospital to ask its state health department to approve an extra 94 beds to ease the overcrowding.
“We don’t have a clear solution,” Raja said.
On Jan. 15, 229 people across the state were boarded and waiting to get a hospital bed, according to the Massachusetts chapter of the ACEP. For comparison, on Jan 17, 2022, during the Covid omicron surge, 278 people were boarded. Neither of those numbers include patients waiting for space to free up on a psychiatric care floor.
Massachusetts is unique in that it keeps very good statistics on the number of people waiting for hospital beds. Many states do not.
Dr. Doug Jeffrey, president-elect of the Texas College of Emergency Physicians, said the situation — which affects ERs across the country — has “gone from our typical organized chaos to an out-of-control crisis.”
“We’re treating people in the waiting room. We’re treating people in the hallways. It’s unsafe for patients,” Jeffrey said.
Michael Day made several trips to the ER before passing away on Aug. 7. While his cancer was terminal, his wife Kathy, who worked 53 years as a nurse, is convinced that his condition worsened because of the delays in care.
“This is not patient care,” Day said. “It’s more like warehousing.”
Hospital care at home
ER boarding has reached such a crisis point that some hospitals have begun to invest in a promising solution to ease the overcrowding crisis.
A federal program called “Acute Hospital Care at Home,” or Hospital at Home, is designed to free up hospital beds, allowing patients to recover in their own beds. It was started by the Centers for Medicare and Medicaid Services in 2020 to help ease hospital strain during the pandemic.
In the program, people who are sick enough to be hospitalized — but well enough to do basic daily activities, such as walk safely to a bathroom — are able to be cared for in their own home, with round-the-clock remote monitoring and twice-daily visits from medical personnel. The average length of “stay” is four days.
Florence Sparks, 80, of Pineville, North Carolina, jumped at the chance to be treated at home rather than stay any longer in an ER. Sparks was having trouble breathing on Jan. 15 and had already spent 17 hours in an emergency department.
Sparks has congestive heart failure — a condition in which the heart doesn’t pump blood effectively — and it was clear that she needed more care than the ER could provide.
Instead of waiting for an in-patient hospital room, her doctors utilized the Hospital at Home program, run by Atrium Health in Charlotte.
A community paramedic checked in on Sparks twice a day, adjusting her IV and her medications as needed — all in collaboration with her doctor.
Atrium Health says it’s managing up to 60 patients a day in North Carolina through its Hospital at Home program, and aims to treat 100 patients daily by the end of 2024. Within the next 18 months, organizers project the program will free up 10% of their in-patient hospital beds.
“If we did not have Hospital at Home, there’s no doubt in my mind, we would have people with longer delays for getting out of emergency departments,” said Matt Anderson, senior medical director, Virtual Health at Atrium. “We know that there’s strain.”
Sparks was able to sleep in her own bed while getting hospital-level care.
“I think they’re more attentive,” she said. “They’re not rushed to see another patient. They give you their undivided attention.”
Colleen Hole, a registered nurse and head of Atrium Health’s Hospital at Home program, called it “the model for the future” and said it could help reduce costs up to 25%.
“It’s proven to be a model that works for our patients and works for our health system capacity challenges,” she said.
At least 311 hospitals in 37 states have been approved to set up the program, although it’s unclear how many are actually using it, according to the Centers for Medicare and Medicaid Services.
CMS funds for the program are set to run out by the end of this year, though Congress could vote to extend it for another two years.
In the meantime, many hospitals have been reluctant to invest resources in it, especially if the funding is uncertain. Hospitals bill CMS directly for Hospital at Home patients on Medicare and Medicaid.
“For many hospitals, it seems like it might not be worth it,” said Nancy Foster, vice president for quality and patient safety policy at the American Hospital Association.
Some private insurers have signed on, but Atrium Health’s Hole said that many of the biggest commercial payers are waiting to see if the federal government continues to fund the program.
While patients languish in ER hallways, waiting for a hospital bed, the federal government has done little else to help.
The Department of Health and Human Services has promised to set up a roundtable within the next six months to “identify actionable next steps and novel opportunities to chart a public-private strategy to address ED crowding and boarding,” HHS Secretary Xavier Becerra wrote in a December 2023 letter to the American College of Physicians.
CMS is scheduled to present national Hospital at Home data to Congress later this year.
“Our hope is that in the final quarter of 2024, we can actually introduce a bill that will become permanent,” Hole said. “I’m anxious because we’re running out of time.”
